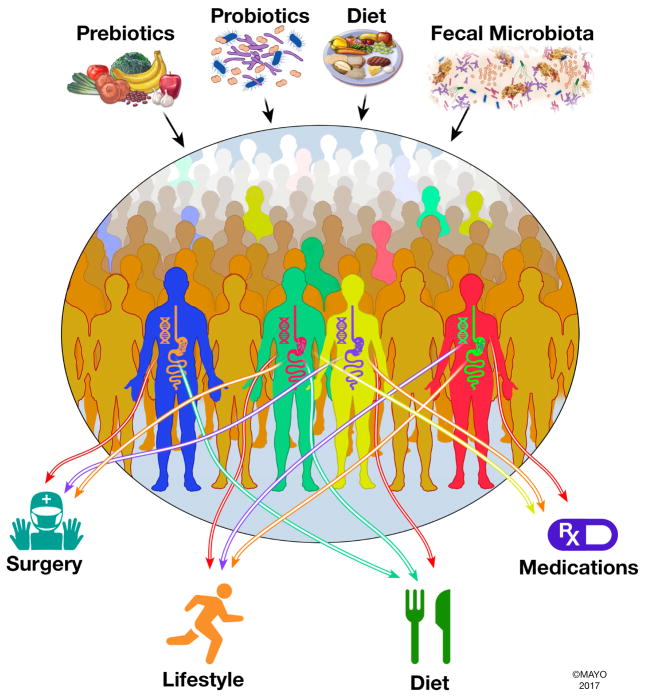
The human microbiome responds to dietary and lifestyle changes, to medications and surgical interventions.
Recently the intestinal microbiome has become a hot topic. It is linked to a variety of diseases and conditions, from diabetes to rheumatoid arthritis to obesity.
- What is the human microbiome?
- How does it affect our health and disease processes?
- Why is the microbiome considered to be at the frontier of personalized medicine?
Let’s explore the answers to these questions.
First of all, we will look at the meaning of the terms related to the microbiome, then review its function. Finally, and most importantly, we will check out biomedical research that may lead to personalized clinical therapies.
Key Terms for Understanding the Human Microbiome
Microorganisms: any organism too small to be seen by the naked eye. Bacteria, viruses, fungi, and protozoa are microorganisms. Also called microbes.
Microbiota: specific community of microorganisms found in a specific environment. The term has been in use for 50 years. Microbiota was formerly called microflora of the gut.
Microbiome: collection of genetic material from all the microbiota. The term was first used as it is defined today in 1988. It is used interchangeably with microbiota, even though there are subtle differences in the meaning of the terms.
Probiotics: live organisms, mostly bacteria, that directly add to the number of healthy microbiotas in the gut.
Prebiotics: non-digestible part of foods that act like fertilizer to stimulate the growth of healthy bacteria in the gut.
What is The Human Microbiota?
Human microbiota refers to the trillions of microorganisms including bacteria, viruses, fungi, and protozoa. They reside primarily in the large intestine (gut) but are also present on the skin and body orifices in much smaller amounts. Interestingly, an individual’s intestinal microbiota can be radically different from that found on the skin.
The human microbiota is associated with chronic diseases such as obesity, inflammatory bowel disease (IBD), diabetes mellitus, atherosclerosis, alcoholic liver disease (ALD), nonalcoholic fatty liver disease (NAFLD), and cirrhosis. The functional role of gut microbes in the development of these diseases remains largely unknown.
Fecal microbiota transplantation (FMT) is a treatment to restore healthy gut microbiota. It involves transplanting stool from a healthy human donor to the patient either by colonoscopy or enema. Patients suffering from C. diff colitis, a debilitating infection resulting from the disruption of microbiota during antibiotic therapy, benefit from this therapy. Although it is not yet possible to tailor the FMT to the individual patient, the success rate for treating C diff colitis is ninety percent.
What is the Human Microbiome?
The human microbiome is the genetic material of all the microbiota – bacteria, viruses, fungi, and protozoa present in the large intestine, skin, or body orifices.
The number of genes in one person’s microbiome is 200 times the number of genes in the human genome. It may weigh as much as five pounds. No two people have the same microbiome. The microbiome was first recognized in the late 1990s.
Microbiome live with humans from birth. It is essential for human development, immunity, and nutrition. The bacteria in the microbiome help digest food and regulate the immune system. Also, it protects against disease-causing bacteria and produces vitamins B12 and K.
Influences that affect the composition of the microbiome are:
- aging
- dietary habits
- treatment with antibiotics and other drugs
- surgery
- disease
- environment
- stress
What is the Role of Prebiotics and Probiotics?
Prebiotics are the non-digestible part of foods (fiber) that are fermented in the large intestine. The fermentation of the fiber feeds beneficial bacteria and helps to increase their numbers. Bananas, onions, garlic, Jerusalem artichoke, apple skins, beans are examples of foods high in prebiotic fiber.
Probiotics differ from prebiotics in that they contain live organisms, mostly bacteria, that directly add to the number of healthy microbiotas in the gut. Foods such as yogurt, sauerkraut, miso soup, and kimchi contain probiotics.
Antibiotic treatment can destroy beneficial bacteria along with the harmful bacteria. To maintain a healthy gut microbiota is important during antibiotic therapy, therefore supplemental probiotics may be recommended.
Health benefits of probiotics and prebiotics have not been proven. However, study of the influence of dietary and supplemental prebiotics and probiotics on the microbiome is currently taking place. This knowledge, plus knowing an individual’s genetic makeup up and that of their microbiome may lead to prescribing probiotics tailored to an individual’s specific need. The FDA has not approved supplemental probiotics.
What Projects are Studying The Human Microbiome?
Human Microbiome Project – National Institutes of Health
Pioneering studies early in 2000 by the National Institutes of Health (NIH) help lay the foundation for the study of the human microbiome. An outgrowth of the study is the Human Microbiome Project (HMP).
The purpose of this 5-yr project is to describe the human microbiome and its role in human health and disease. If the project succeeds in defining microbiome changes associated with diseases and how to alter microbial distortions, it may transform medicine.
Mayo Clinic Center for Individualized Medicine Microbiome Program
The intestinal microbiome is being studied the most. It is by far the largest, is easy to access. Understanding the intestinal microbiome may have the greatest impact on improving health through the new frontier of personalized medicine. Mayo Clinic Center for Individualized Medicine Microbiome Program is studying just that. Its purpose is to seek an understanding of how the microbiome promotes wellness and how disruption of the microbiome (dysbiosis) can enable disease. Disorders currently under study at Mayo Clinic are gluten sensitivity, C. diff infection, rheumatoid arthritis, colon cancer, and bacterial vaginitis.
A Video from Mayo Clinic Radio on The Microbiome
What Does the Future Hold?
Human gut microbiota in health and disease is beginning to be understood. We know the microbiome can be modified or changed by different treatments, whereas, the body genes cannot. In addition, once more is understood about the diversity of microbes and their role in health and disease, manipulating the microbiome may lead to personalized medical treatment. Consequently, we may see probiotics, diet, and fecal microbiota transplants tailored to an individual’s specific need. This is why microbiota is considered to be at the frontier of personalized medicine.
References
https://www.mayo.edu/research/centers-programs/center-individualized-medicine/research/translational-programs/microbiome
https://microbiomejournal.biomedcentral.com/articles/10.1186/s40168-019-0620-y
https://www.mayo.edu/research/centers-programs/center-individualized-medicine/research/translational-programs/microbiome
https://www.mayoclinic.org/healthy-lifestyle/consumer-health/expert-answers/probiotics/faq-20058065
https://www.sciencedirect.com/science/article/pii/S2095809917301492