Lyme Disease: The Most Common Vector-Borne Disease in the United States
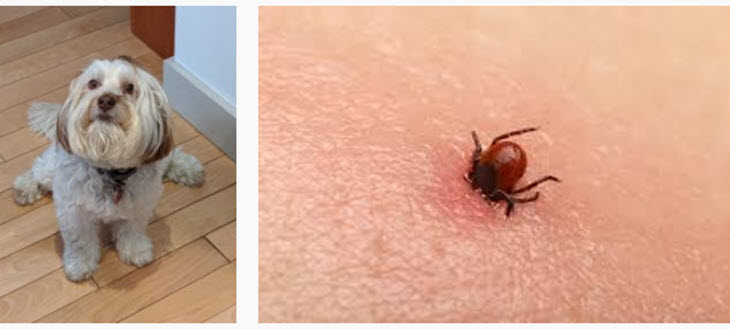
As I removed six ticks from our dog, Bentley, the other day, it reminded me that May is Lyme disease month and time to review how to avoid getting it for another year.
What is Lyme Disease?
Lyme disease is an infection caused by Borrelia burgdorferi bacteria. The bacteria are transmitted to humans through a bite from a blacklegged tick (deer tick), which becomes infected from feeding on deer or mice (vectors).
The bacteria eventually find their way into the bloodstream. Only a minority of blacklegged tick bites lead to Lyme disease.
According to the Centers for Disease Control and Prevention (CDC), approximately 30,000 cases of the disease are reported each year. It was first described in 1975 when unusually large numbers of children were diagnosed with juvenile rheumatoid arthritis in and near Lyme, CT.
Medical Terminology Tips
Use these tips to help navigate the information below
Lyme disease: An eponym named after Lyme, CT. When using the term, Lyme is capitalized and disease is not, as in Lyme disease.
Bell palsy: The modern trend for medical terminology is to use the non-possessive form of eponyms as in Bell palsy instead of Bell’s palsy. The ‘p’ in palsy remains lowercase.
Blacklegged vs. black-legged: Both spellings are acceptable. It appears that blacklegged is the more common spelling when used in medical writings.
Vector-born vs. zoonotic: Zoonotic diseases are diseases of animals that can be transmitted to humans. Many zoonotic diseases require a vector (such as deer or mice) in order to be transmitted from animals to humans. COVID-19 is a vector-borne disease.
Borrelia burgdorferi: (bu-REL-ee-a) (burg-dor-FRE-i) The name of the bacteria that causes Lyme disease. It is named after its discoverer, Dr. Willy Burgdorfer; Borrelia is the name of the type of bacteria.
Erythema migrans (er-a-THEE-ma) (MY-grans) A circular red rash.
The Disease
- Symptoms and signs of the disease can occur anywhere from 3 to 30 days after the bite, or they can appear even months later, depending on the stage of the infection.
- Ticks must be attached for 36 to 48 hours in order to transmit Lyme disease. Most infections can be successfully treated with antibiotics.
- If left untreated, the infection can spread to the joints, heart, and nervous system.
Three Stages of the Disease
The disease can generally be divided into three phases: early localized, early disseminated, and late disease. The signs and symptoms of each stage can overlap. Some patients may present with a later-stage disease without experiencing the earlier phase signs and symptoms.

Early localized disease starts one to two weeks after the tick bite. The bacteria are localized. Erythema migrans, a circular red rash, usually appear at the site of the bite within 7-10 days. It is not always present.
Other signs and symptoms may appear, including the following:
- Fatigue
- Anorexia (loss of appetite)
- Headache
- Arthralgia (pain in a joint)
- Myalgia (muscle pain)
Early disseminated disease occurs weeks to several months after the tick bite when bacteria have spread throughout the body. Cardiac and neurological involvement is often present. Symptoms and signs may include:
- Flu-like symptoms – chills, fever, fatigue, headache, and joint pain
- Bell palsy (facial paralysis)
- Meningitis (inflammation of the membrane covering the spinal cord and brain)
- Arthralgia (pain in the joint)
- Neuropathy (disease of the nerve)
- Radiculopathy (disease of the nerve roots)
- Arrhythmias (disturbance of the rhythm of the heart)
Late disease occurs when the infection isn’t treated during phases 1 or 2 of the disease and can occur months or years after the tick bite. The bacteria have spread throughout the body. Symptoms and signs may include:
- Arthritis (inflammation of the joints)
- Fibromyalgia (muscle and soft tissue syndrome)
- Encephalopathy (cognitive disturbances such as short-term memory loss, difficulty concentrating, and problems following conversations)
- Polyneuropathy (disease of many nerves)
Diagnosis
Laboratory tests to identify antibodies to the bacteria can help confirm or rule out the diagnosis. These tests are most reliable a few weeks after infection. They include an enzyme-linked immunosorbent assay (ELISA) test to detect antibodies to B. burgdorferi. If the ELISA test is positive, a western blot test is usually done to confirm the diagnosis.
Laboratory tests are not recommended for patients who do not have symptoms typical of the disease.
Treatment
Oral antibiotics are used to treat Lyme disease. In general, recovery will be quicker and more complete the sooner treatment begins. People treated with appropriate antibiotics in the early stages of the disease usually recover rapidly and completely.
If not appropriately treated, the disease can progress to early disseminated and late disease.
Awareness
May is Lyme Disease Awareness Month. Most identified cases of Lyme disease occur during June, July, and August, and right now is the best time to learn how to avoid tick bites and what to do if you are bitten.
Use these two websites to learn more: Preventing Tick Bites on People and Tick Removal and Testing.
Have a safe summer!
Visual Recap
Watch this 2-minute video to review the signs and symptoms of Lyme disease.
Watch this 3-minute video on Lyme disease and Borrelia burgdorferi.
Medical term definitions: Exploring Medical Language 11 Edition
References:
Online UpToDate
https://dph.georgia.gov/zoonoticvector-borneinfestations
https://www.medicinenet.com/script/main/art.asp?articlekey=31967
https://www.cdc.gov/lyme/index.html